What role do hormones play in PCOD treatment?
Introduction
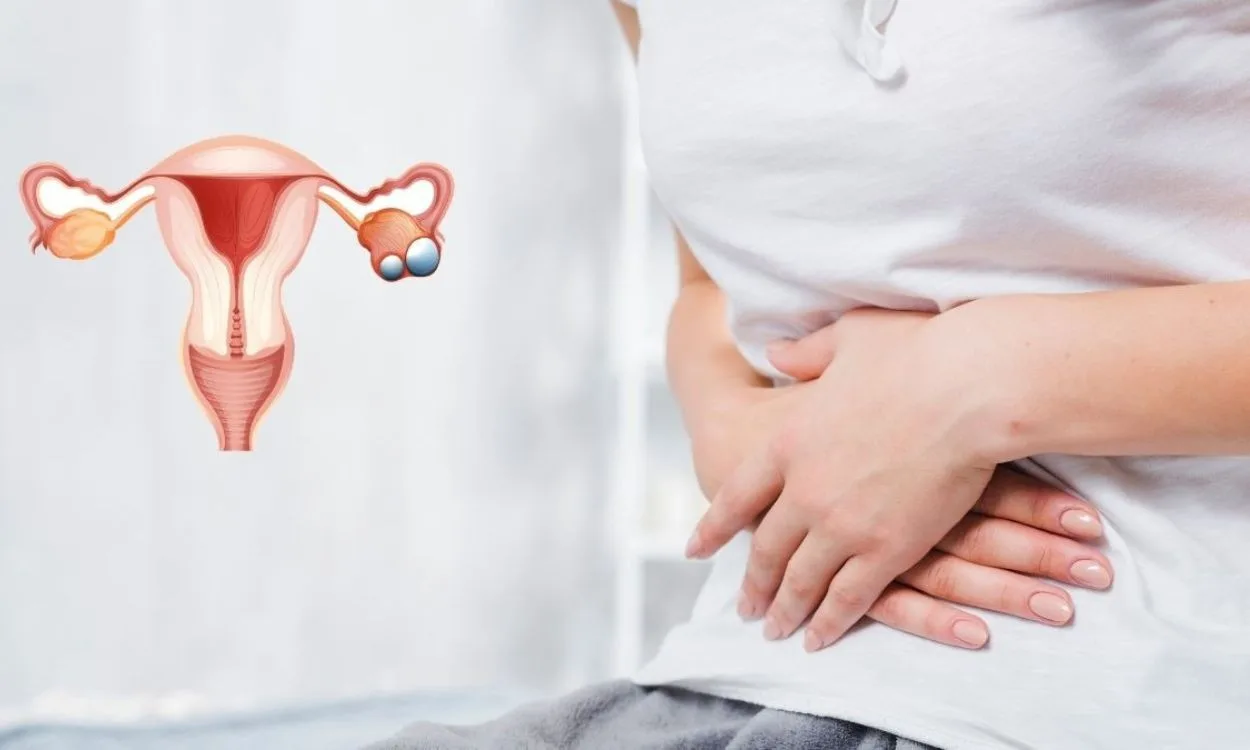
Polycystic Ovary Syndrome (PCOS) is a common hormonal disorder that affects women of reproductive age. It is characterized by an imbalance of hormones, specifically elevated levels of androgens (male hormones) and insulin. PCOS can lead to a variety of symptoms and long-term health complications if left untreated. Understanding the role of hormones in PCOS is crucial for effective treatment and management of this condition.
Hormones involved in PCOS
- Androgens: Androgens are male hormones that are present in both males and females. In women with PCOS, there is an overproduction of androgens, such as testosterone, which can cause symptoms like excess hair growth (hirsutism), acne, and male-pattern baldness.
- Insulin: Insulin is a hormone that regulates blood sugar levels. In PCOS, the body becomes resistant to insulin, leading to elevated levels of insulin in the blood. This can contribute to weight gain and difficulty in losing weight, as well as an increased risk of developing diabetes.
- Estrogen and Progesterone: Estrogen and progesterone are female hormones that play a crucial role in regulating the menstrual cycle. In PCOS, there is an imbalance of these hormones, leading to irregular or absent periods.
- Luteinizing Hormone (LH): LH is a hormone that stimulates the ovaries to produce and release eggs. In women with PCOS, there is an increased production of LH, which can disrupt the normal ovulation process and contribute to infertility.
Impact of hormone imbalance in PCOS
The hormonal imbalances in PCOS can have various effects on the body and contribute to the symptoms and complications associated with this condition:
- Irregular menstrual cycles: The imbalance of estrogen and progesterone can disrupt the normal menstrual cycle, leading to irregular or absent periods.
- Ovarian cysts: The elevated levels of LH can cause the ovaries to produce excess amounts of androgens, leading to the formation of small cysts on the ovaries. These cysts can interfere with normal ovulation.
- Infertility: Due to the disruption of ovulation and irregular menstrual cycles, women with PCOS may experience difficulties in getting pregnant.
- Weight gain and difficulty in losing weight: Insulin resistance and elevated androgen levels can contribute to weight gain and make it harder for women with PCOS to lose weight.
- Acne and hirsutism: The excess production of androgens can contribute to the development of acne and excessive hair growth in areas typically associated with males (like the face, chest, and abdomen).
PCOS treatment and hormone regulation
The treatment of PCOS aims to address the hormonal imbalances and manage the associated symptoms. Here are some strategies commonly used:
- Lifestyle modifications: Making changes to diet and exercise habits can help improve insulin sensitivity and manage weight. A balanced diet with a focus on whole foods, regular physical activity, and stress management techniques can be beneficial.
- Medications: Hormonal birth control pills can help regulate the menstrual cycle and reduce androgen levels. Anti-androgen medications may also be prescribed to manage symptoms like hirsutism and acne. Insulin-sensitizing drugs like Metformin can help improve insulin resistance.
- Fertility treatments: For women trying to conceive, medications like Clomiphene or Letrozole may be prescribed to stimulate ovulation. In more severe cases, assisted reproductive technologies like in vitro fertilization (IVF) may be recommended.
- Weight management: Achieving and maintaining a healthy weight can help regulate hormones and improve symptoms. This can be achieved through a combination of diet, exercise, and behavioral changes.
Fitpaa: Supporting PCOS treatment and management
Fitpaa is an AI-driven health and fitness app that can be a valuable tool in the treatment and management of PCOS. Here’s how Fitpaa can support women with PCOS on their journey:
- Metabolism monitoring: Fitpaa’s Metabolism Assessment can help identify the underlying factors contributing to PCOS by assessing the individual’s current metabolism. This information can guide personalized treatment plans.
- Expert guidance: Fitpaa provides access to expert fitness coaches, nutritionists, and doctors who can develop a personalized Fitpaa Capsule based on the individual’s metabolism, health goals, and lifestyle. This capsule combines medical therapy, exercise therapy, nutrition therapy, and cognitive behavioral therapy to optimize metabolism and achieve health and fitness goals.
- Real-time guidance and tracking: Fitpaa’s Realtime Guidance technology incorporates habit-building techniques and timely nudging to keep users motivated and on track. The Fitpaa mobile app offers features like virtual workout trainers, diet tracking, performance tracking, and progress tracking to support adherence to the personalized Fitpaa Capsule.
- Regular reviews and course corrections: Fitpaa’s team of fitness planners, nutritionists, fitness trainers, and doctors review progress regularly and make necessary adjustments to the Fitpaa Capsule to ensure optimal results.
In conclusion, hormones play a significant role in the development and management of PCOS. Understanding the hormonal imbalances and addressing them through a comprehensive treatment plan can help alleviate symptoms, improve fertility, and support overall health. Fitpaa, with its personalized approach and advanced technology, can be a valuable tool in the treatment and management of PCOS, empowering women to achieve their health and fitness goals with guaranteed results.
Download the Fitpaa app
Experience the joy of achieving your health and fitness goals with the help of Fitpaa’s all-in-one health and fitness platform. Download the Fitpaa app now and start your journey towards a healthier, happier life. Fitpaa’s personalized approach and expert guidance will support you every step of the way. Remember, your well-being is our mission!
Note: Fitpaa is a paid service, but it offers a 7-day risk-free trial and a money-back guarantee if the promised results are not achieved.